
Provider Reference Manual
Select Health Pharmacy Plans
March 2024

2
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Table of Contents
1.0 General Overview ................................................................................................................................................. 4
1.1 Confidentiality Statement ..................................................................................................................................... 4
1.2 Pharmacy Requirements ....................................................................................................................................... 4
2.0 Contact Information ........................................................................................................................................... 6
2.1 Select Health Pharmacy Help Desk .................................................................................................................. 6
2.2 Prior Authorization Requests ............................................................................................................................... 6
2.3 Select Health Member Services ......................................................................................................................... 6
2.4 Select Health Addresses ........................................................................................................................................ 6
3.0 General Claims Processing Information .........................................................................................................7
3.1 Online Processing Information .............................................................................................................................7
3.2 Select Health ID Cards .............................................................................................................................................7
3.3 Member Identification Number ...........................................................................................................................7
3.4 Dependent Coverage .............................................................................................................................................. 8
3.5 Eligibility Verification ............................................................................................................................................... 8
3.6 Coordination of Benefits ........................................................................................................................................ 8
3.7 Prescription Costs and Reimbursement ......................................................................................................... 9
3.8 Signature Log ........................................................................................................................................................... 10
3.9 EPrescribing ............................................................................................................................................................ 10
4.0 Dispensing Edits ................................................................................................................................................. 11
4.1 Quantity and Day Supply Limits ..........................................................................................................................11
4.2 Refills .............................................................................................................................................................................11
4.3 DAW Codes ................................................................................................................................................................12
4.4 Compound Prescriptions ...................................................................................................................................... 12
5.0 Appeals and Grievances .................................................................................................................................... 14
5.1 Member Appeals and Grievances .....................................................................................................................14
5.2 MAC Pricing Research Requests ....................................................................................................................... 14
5.3 Pharmacy Appeals ..................................................................................................................................................14
6.0 Audit Information................................................................................................................................................15
7.0 Formulary Information .......................................................................................................................................16
7.1 Select Health Commercial and Scripius PBM Products .............................................................................16
7.2 Select Health Medicare (Medicare Part D) ..................................................................................................... 18
7.3 Select Health Community Care (Medicaid) ...................................................................................................19
8.0 Common Reject Messages ..............................................................................................................................21
9.0 Payment and Reconciliation Information ....................................................................................................24
Continued on page 3....

3
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
9.1 Payment Schedule ..................................................................................................................................................24
9.2 Remittance Report ................................................................................................................................................24
9.3 Electronic Funds Transfer (EFT) ........................................................................................................................24
9.4 340B Claims .............................................................................................................................................................24
10.0 Select Health Medicare (Medicare Part D): Specific Information ........................................................25
10.1 Plan Summary .........................................................................................................................................................25
10.2 Fraud, Waste, and Abuse ...................................................................................................................................25
10.3 Training .....................................................................................................................................................................25
10.4 Pharmacy Certification for Part D .................................................................................................................. 25
10.5 Federal Health Care Programs Participation Exclusion ........................................................................25
10.6 General Procedures for Acknowledgment Letters ..................................................................................25
10.7 Formulary Transition Fill Plan ...........................................................................................................................25
10.8 Long-term Care (LTC) Facilities ....................................................................................................................... 26
10.9 Home Infusion Therapy ...................................................................................................................................... 26
10.10 Medicare Service Area ......................................................................................................................................26
11.0 Select Health Community Care (Medicaid): Specific Information ........................................................ 27
11.1 Tamper-Resistant Prescription Pad Requirements ................................................................................... 27
11.2 Generic Preparations ...........................................................................................................................................27
11.3 Medications Provided in a Medical Emergency .........................................................................................27
11.4 Restriction Program .............................................................................................................................................27
Appendix: Payer Sheet ............................................................................................................................................29
Table of Contents, Continued

4
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
This pharmacy provider manual has been developed by Select Health/Scripius to assist
network pharmacies in all aspects of providing pharmacy services to covered members.
Periodically, this manual will be updated with new or modified information. To ensure
accuracy and usability of this manual, please incorporate the revised information as
instructed. This manual has been assembled to provide administrative information only
and is not meant to supersede any local or federal regulations.
Select Health/Scripius administers a variety of plans including Commercial, Small
Employer, Individual, Medicaid, Medicare, and other Government sponsored plans.
The Select Health pharmacy network is comprised of nationally contracted chain
and independent pharmacies located in all 50 states. Covered members with Select
Health prescription drug coverage must have their prescriptions filled at a participating
pharmacy to obtain the maximum benefit. Covered members traveling outside their local
service area must also use a participating pharmacy to obtain the maximum benefit.
Pharmacies participating in the Select Health pharmacy network are eligible to fill
prescriptions for Select Health plans and/or lines of business identified in the pharmacy
network agreement, unless participation is restricted by the plan. For some plans, the
prescriber writing the prescription must be participating in the plan.
The information included in this provider manual is considered confidential and
proprietary to Select Health and provided for business purposes only. Provider is not
authorized to copy, reproduce, distribute, or otherwise share the information contained in
the manual except as authorized by the pharmacy network agreement.
Select Health has established service, credentialing, and operational standards for
participating pharmacies to ensure delivery of quality service to all covered members.
Patient service standards include that pharmacies/pharmacists will:
• Maintain patient profiles for prescription medication dispensed.
• Not destroy any patient record produced, unless prior written consent is obtained
from Select Health, for a period of at least five (5) years.
• React appropriately to online edits, which may affect the patient’s medical status or
coverage.
• Provide instruction to the patient on the use of medication, including information
based on the online drug messages, before dispensing of each prescription,
according to state and federal law.
• Provide all drug products covered by the benefit plans, including products normally
stocked and those that require special order, if possible.
• Have established formal prescription quality assurance and error prevention measures.
• Have a formal process for handling prescription errors.
1.1 CONFIDENTIALITY
STATEMENT
1.0 General Overview
1.2 PHARMACY
REQUIREMENTS
For any questions or issues
not resolved in this provider
manual, please email
SHPharmacyContracting@
selecthealth.org.

5
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Provider credentialing standards include that the pharmacy will:
• Carry a valid pharmacy operating license.
• Maintain valid professional liability and general liability insurance for the pharmacy in
the amounts of $1,000,000 per occurrence and $3,000,000 aggregate coverage.
• Maintain a valid DEA registration.
• Cooperate with Select Health pharmacy auditors and recovery of any overages
identified as a result of an audit.
• Maintain a current/valid State Board of Pharmacy License that contains no
restrictions (established procedures for verification of pharmacist licensure will be in
place).
Contact the Pharmacy Help Desk for items such as the following:
• Claims Processing
• Prior Authorization Requests
• Assistance with Reject Messages (see Section 8.0)

6
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Contact the Help Desk for:
• Network and Contract Issues/Questions
• Claims Investigation
• Provider Remittance Statements
• Payment Issues/Questions
• General Questions
Help Desk Phone Numbers:
• Select Health Commercial
Scripius PBM Products
Select Health Community Care
®
(Utah State Medicaid)
— Toll Free: 8004429988
— Fax: 8014423006
Electronic prior authorization requests can be submitted using most electronic medical
record platforms, or via https://selecthealth.org/pa.
Contact the relevant Member Services line listed below for eligibility verification or
member-specific questions about benefit coverage:
• Select Health Commercial Products
— Toll Free: 8005385038
— Fax: 8016503279
• Select Health/Scripius PBM Products
— Toll Free: 8004423127
— Fax: 8014423006
Physical Address: 5381 Green Street, Murray, UT 84123
Claims Mailing Addresses:
• Commercial, Scripius PBM, and
Select Health Community Care (Medicaid)
— PO Box 30192
— Salt Lake City, UT 84130
2.0 Contact Information
2.1 SELECT HEALTH
PHARMACY
HELP DESK
24 hours a day,
7 days a week
2.3 SELECT HEALTH
MEMBER
SERVICES
Monday through Friday,
7:00 a.m.–9:00 p.m.
(MST)
Saturday, 9:00 a.m.–
3:00 p.m. (MST)
Closed Sunday
• Select Health Medicare
(Medicare Part D)
— Toll Free: 8554429900
— Fax: 8016503170
• Select Health Community Care
(Medicaid)
— Toll Free: 8554429900
— Fax: 8668114997
2.4 SELECT HEALTH
ADDRESSES
2.2 PRIOR
AUTHORIZATION
REQUESTS
• Select Health Medicare
®
(Medicare Part D):
— Toll Free: 8554429988
— Fax: 8014420413
• Select Health Medicare
(Medicare Part D)
— PO Box 30196
— Salt Lake City, UT 84130

7
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
3.0 General Claims Processing Information
• Select Health Commercial and Scripius PBM Products
— BIN 800008
— PCN – not required
— Group – not required
• Select Health Medicare (Medicare Part D)
— BIN 015938
— PCN 7463
— Group – UT/ID/CO = U1000009; NV Intermountain = U1000011
• Select Health Community Care (Utah State Medicaid)
— BIN 800008
— PCN 606
— Group – not required
The pharmacy must submit all prescription claims online to Select Health using the
most current version of the NCPDP telecommunications standard. Tape billing will not
be accepted or paid. The pharmacy must submit prescription claims within 90 days of
the fill date. The pharmacy is required to bill the most cost-effective package size.
Each individual claim will be processed as received by Select Health. Extensive edit
checks are made to ensure proper claims adjudication. Claims submitted containing
one or more errors will be rejected.
The pharmacy shall not submit claims for payment for prescriptions filled, but not
dispensed to a covered member. Non-compliance with this contractual provision will
be grounds for termination of the Prescription Drug and Pharmacy Services Agreement
and/or adjustment of payment on these claims.
Select Health maintains a guide with sample ID cards on their website. The primary
cardholder of Select Health will receive an ID card that will provide the cardholder’s
identification number and copayment information.
The identification number will appear as follows: 800000000 (example).
Select Health Community Care Identification Numbers
Individuals enrolled in Select Health Community Care will be issued a Select Health
identification number upon enrollment. The Utah Department of Health will continue to
issue Medicaid identification cards. Pharmacies should request both the Select Health
and Medicaid cards when dispensing medication.
Select Health Community Care claims can be submitted for processing using either the
Select Health or Medicaid identification number.
3.1 ONLINE
PROCESSING
INFORMATION
See Appendix: Payer
Sheet beginning
on page 29 for
additional processing
instructions and
requirements.
3.2 SELECT HEALTH
ID CARDS
3.3 MEMBER
IDENTIFICATION
NUMBER

8
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
3.4 DEPENDENT
COVERAGE
Dependent coverage may include a spouse and/or children. Covered family members
are identified by the following relationship codes:
0 Not Specified
1 Cardholder
2 Spouse
3 Child
4 Other
NOTE: Use of the correct relationship code is important. Prescription claims must be
submitted to Select Health only for the eligible member for whom the prescription is
written by the prescriber. This requirement has added significance in that DUR reviews
are based on claims submitted for the correct eligible member.
The pharmacy agrees to use an online point-of-sale (POS) authorization terminal or
host-to-host online link with the Select Health system for verifying eligibility of covered
members. The cardholder’s identification number for POS entry should be obtained
from their ID card. These cards are used for identification purpose only and are not a
guarantee of coverage.
If eligibility cannot be verified using the above method, the pharmacy should call the
Select Health Pharmacy Help Desk for verification of eligibility using the telephone
number listed on the identification card. Select Health will advise the pharmacy if the
patient is eligible.
Select Health Community Care members must use a participating pharmacy of Utah
Medicaid and Select Health Community Care to obtain benefits.
Members not using a participating pharmacy must pay in full for their prescription(s)
and seek reimbursement from Select Health.
Members will be reimbursed the discounted amount that the plan would have had
to pay to a participating pharmacy for the prescription(s), less the copayment. For
Medicare, Select Health Medicare will only cover up to a 30-day supply at an out-of-
network pharmacy. The member will be reimbursed for Part D medications covered on
the plan’s Drug List (formulary) that were not paid for with assistance from a discount
or coupon card.
Most Select Health plans allow for coordination of benefits (COB) with a member’s
primary carrier. If a member has an additional prescription benefit plan, the pharmacy
should submit the claim to the appropriate payer in accordance with any coordination
of benefits requirements. The pharmacy should submit the primary claim to the
member’s primary payer for adjudication. In some instances, the secondary claim
can be electronically submitted to Select Health for adjudication. The member may
5 Student
6 Disabled Dependent
7 Adult Dependent
8 Significant Other
3.5 ELIGIBILITY
VERIFICATION
3.6 COORDINATION OF
BENEFITS COB

9
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
seek reimbursement from Select Health for any secondary claims not processed
electronically.
Secondary Claim Submission (Select Health Community Care)
Pharmacies must explore payment from all other liable parties such as insurance
coverage, including a health plan, before seeking Medicaid payment. Before submitting
a secondary claim to Select Health Community Care, collect only the applicable
Medicaid copayment usually charged at the time of service. Refer to Utah Medicaid
Provider Manual, Section 1, Chapter 11.4 for additional instruction regarding
coordination with other liable parties.
Member Financial Responsibility
When a person presents a Select Health ID card to the pharmacy, the ID card may
advise of the copayment amount to be collected. Since the pharmacy is submitting the
claim via the point-of-sale system, the electronic response to the pharmacy will include
a detailed description of the member’s financial responsibility.
If the member is questioning the calculated copay or coinsurance amounts returned on
the transaction, remind the member that the copay is determined by many factors. The
following is a non-inclusive list of items that may affect the copayment or coinsurance
being returned:
• Brand vs. Generic Drug
• Quantity Dispensed
• Day Supply Dispensed
• Member Deductible
If a review of the above items still leaves questions for the member regarding their
calculated copay, direct the member to contact the Select Health Member Services line
for assistance.
Prohibition on Billing Patients
Participating pharmacies of Select Health/Scripius are prohibited to collect payment
from members, for covered services, that exceeds the copay or coinsurance amount
returned via the point-of-sale system. This includes, but is not limited to, any amount
less than the pharmacy’s acquisition cost, any additional cost incurred when a specific
brand or manufacturer is requested by the member, additional fees for services
included in the dispensing of the drug (i.e. additional compounding fees), etc.
Participating pharmacies of Utah Medicaid and Select Health Community Care are
only allowed to collect payment from Medicaid enrollees for non-covered services
when certain circumstances are met. The specific policy is described in the Utah
Medicaid provider manual. See the Utah Medicaid Provider Manual, Section 4.
3.7 PRESCRIPTION
COSTS AND
REIMBURSEMENT

10
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Reimbursement Rate Questions
If the pharmacy has questions regarding the reimbursement rate for a particular
medication, they are welcome to contact the Select Health Pharmacy Help Desk for
assistance. Additionally, the pharmacy can review the following items that can directly
affect the reimbursement rate to ensure the transaction was submitted correctly:
• Quantity Submitted: Confirm that the metric quantity of the prescription was
submitted correctly.
• Day Supply: Confirm that the day supply of the prescription was submitted correctly.
• DAW Code: Confirm that the submitted DAW code accurately reflects the situation.
After evaluating the above fields, if all appears to be accurate, call the Select Health
Pharmacy Help Desk for further assistance.
The pharmacy will maintain an approved daily signature log which contains a
disclaimer verifying the member has received the prescription and authorizes the
release of all prescriptions and related information to Select Health. The pharmacy will
also require the member or the representative who receives the service to sign for all
prescriptions dispensed.
Electronic prescribing (e-prescribing) is the transmission, using electronic media, of
prescription or prescription-related information between a prescriber, dispensing
pharmacy, pharmacy benefit manager, or health plan, either directly or through an
intermediary. E-prescribing should improve quality, safety, efficiency, and consumer
convenience.
Pharmacies must submit the Origin Code on the transaction, in accordance with the
Payer Sheet included in this Provider Manual, to indicate how the prescription was
obtained by the pharmacy.
To qualify as an electronic prescription, the electronic prescription must be noted prior
to dispensing, and must clearly record, in a manner that cannot be altered, the system-
assigned user and date and time stamp to take the place of hard copy documentation.
For auditing purposes, the following data elements should be present on an electronic
prescription as authentication of electronic signatures:
• Electronic Transaction Identifier
• Prescriber Identifier(s)
• Written Date/Time
• Designated Agent (if applicable)
Pharmacies may only dispense federally Controlled Substances based on a written
or electronic prescription that complies with all applicable laws and regulations for
prescribing and dispensing Controlled Substances.
3.8 SIGNATURE LOG
3.9 EPRESCRIBING

11
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
4.0 Dispensing Edits
This section contains information on some of the more common edits applied to the
Select Health plans.
Select Health Commercial, Scripius PBM Products, and Select Health
Community Care (Utah State Medicaid)
The following quantity limits will be applied to all transactions processed to Select
Health:
• Maximum thirty-four (34)-day supply of tablets, capsules, and liquids to be taken orally.
• Maximum one (1) vial containing no more than fifteen (15) milliliters of any otic or
ophthalmic product; if only manufactured in package sizes greater than fifteen (15)
milliliters, the smallest package size available from the manufacturer is mandated. One
copay will be charged per vial.
• Some products may be limited to an approved quantity per each acute treatment
period.
Unless otherwise specified, one copayment will apply for each item dispensed within
the limit. There are instances in which exceptions can be made.
Except for Select Health Community Care (Medicaid), most Select Health plans offer
a ninety (90)-day supply benefit for maintenance medications, if the member and
medication meet specific qualifications. The necessary qualifications include that the
medication must be approved on the formulary, and the member must have filled
the prescription, at the same strength, at least once within the past 180 days. If the
pharmacy has questions regarding eligibility or if a rejection is received when the claim
is processed, please contact the Pharmacy Help Desk for assistance.
Select Health Medicare (Medicare Part D)
For certain drugs, the Medicare plan may limit the amount of a prescription a member
can receive (maximum number of tablets or capsules, etc. per prescription). Asking for
an exception may allow for greater quantity dispensed when a medication exceeds the
plan limits.
The following refill edits will be applied to all transactions processed to Select Health:
• Prescriptions cannot be refilled beyond twelve (12) months from the date on which
the prescription was written. After the 12 months have lapsed, a new prescription
with a new prescription number must be assigned.
• Prescriptions should not be refilled more times than the number specified by the
prescriber.
• Additional refills authorized by the prescriber must be documented on the hard copy
of the prescription or a new prescription number must be assigned with the refills
indicated.
4.1 QUANTITY AND
DAY SUPPLY
LIMITS
4.2 REFILLS

12
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
• Changes in dosage or an increase in quantity assigned by the prescriber must be
documented on the hard copy prescription or a new prescription number must be
assigned with these changes documented.
Pharmacies that do not comply with the above dispensing limitations
may be subject to review by the Select Health Pharmacy auditors or designated vendor.
The pharmacy is required to bill the correct Dispense as Written (DAW) code
corresponding to the prescription. Valid DAW codes are as follows:
DAW Code Code Description
0 No product selection indicated
1 Substitution not allowed by prescriber
2 Substitution allowed – patient requested product dispensed
3 Substitution allowed – pharmacist selected product dispensed
4 Substitution allowed – generic drug not in stock
5 Substitution allowed – brand drug dispensed as generic
6 Override
7 Substitution not allowed – brand drug mandated by law
8 Substitution allowed – generic drug not available in marketplace
9 Other – not a valid code for Select Health
Compounded prescriptions must be prepared following good compounding practices
as defined by the United States Pharmacopoeia (USP DIVolume III: Approved Drug
Products and Legal Requirements). The pharmacy will follow USP good compounding
practices concerning the following:
• Facility space and equipment
• Source ingredient selection and calculations
• Stability, sterility, and beyond-use dating
• Formulation and checklist for acceptable strength, quality, and purity
• Compounding log and quality control
Formulation records, compounding logs, and quality control records may be subject to
review by the Select Health Pharmacy Auditors or designated vendor. Claim dollars for
compounded prescriptions found not following good compounding practices will be
subject to adjustment.
All active ingredients in a compounded prescription must be FDA-approved for human
use and must be covered under the member’s plan. The Select Health Pharmacy Help
Desk is available to assist in determining a member’s coverage. Dispensing quantity
limitations apply to all covered compounded prescriptions (see “Quantity Dispensed”
section).
4.3 DAW CODES
4.4 COMPOUND
PRESCRIPTIONS
NOTE: Compounds
are not covered for
all plans or lines of
business.

13
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
In accordance with NCPDP version D.0 as mandated by HIPAA 5010, Select Health
processes multi-ingredient compounds. Each NDC should be included in the
compound segment of the transaction. Refer to the Select Health payer sheet in
appendix A for additional requirements. Compounded prescriptions where the
reimbursement due to the pharmacy exceeds $75.00 will require a review from the
Select Health Pharmacy Help Desk and an official prior authorization request may be
required.
Non-Covered Ingredients
The cost of non-covered ingredients may not be billed or collected from an enrollee of a
Select Health plan when there are covered ingredients of the compound.

14
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
5.0 Appeals and Grievances
Select Health Commercial, Select Health/Scripius PBM Products, and
Select Health Community Care (Utah State Medicaid)
Please direct all appeals or grievances on behalf of a member, to the Select Health
Member Appeals department, by phone or in writing to:
Select Health
Attn: Member Appeals Department
P.O. Box 30192
Salt Lake City, UT 84130
Phone: 8442089012
Fax: 8014420762
Email: [email protected]
Select Health Medicare (Medicare Part D)
A grievance is an escalated complaint from a Medicare member regarding a specific
issue as it relates to the service they received. For example, an official grievance is
not filed over specific formulary rules or plan costs, but rather would be related to
the timeliness of filling a prescription or if the member received other poor service.
Members are welcome to contact Select Health through the Medicare Member
Services line, fax line, or through U.S. mail.
Pharmacies who disagree with the MAC pricing on a claim may submit a MAC
Pricing Research Request (dispute) through Select Health’s online tool available at
selecthealth.org/pharmacy/resources.
Requests must be received within 21 days of initial adjudication. Additionally, an invoice
dated within 30 days of the claim’s date of service, showing the pharmacy’s acquisition
cost, must be provided. Requests outside of these parameters or sent via email will not
be accepted.
For any escalated questions or issues not resolved in this provider manual, pharmacies
may email concerns to SHPharmacyContrac[email protected].
5.1 MEMBER APPEALS
AND GRIEVANCES
5.2 MAC PRICING
RESEARCH
REQUESTS
5.3 PHARMACY APPEALS

15
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
6.0 Audit Information
Select Health or designated vendor regularly monitors and audits pharmacy claims.
Part of this process is accomplished by the pharmacy providing access at reasonable
times upon request by either Select Health or their designee or any governmental
regulatory agency to inspect the facilities, equipment, books, and records of the
pharmacy. This includes, but is not limited to, member records and all prescription
dispensing records. A notice will be sent to the pharmacy location that has filled the
prescription(s) in question. A description of the issue under review will be included,
along with specific claim-related information.
The pharmacy is given thirty (30) days from the date of the letter to respond,
depending on the scope of the audit. If a response is not received within this period, this
will be interpreted as non-compliance and the pharmacy is subject to adjustment of
the paid dollars on those claims.
Additionally, when billing discrepancies are identified by Select Health and are
disclosed to the pharmacy, the pharmacy is given thirty (30) days to review/dispute
the findings. If a response is not received within this time, this will be interpreted as
consent to the finding and the adjustments will be reflected on the pharmacy’s next
remittance cycle.
When necessary, extensions will be granted if the pharmacy contacts Select Health
within the specified time.

16
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
7.0 Formulary Information
7.1 SELECT HEALTH
COMMERCIAL AND
SCRIPIUS PBM
PRODUCTS
NOTE: Compounds
are not covered for
all plans or lines of
business.
Covered Medications and Services
Covered prescription drugs and pharmacy services include most medications which
require a prescription by state or federal law when prescribed by a physician and
listed on the Select Health drug formulary. Among other medications, this includes the
following:
• Injectable insulin and insulin syringes when written on a prescription
• Compounded medications that are prepared following good compounding practices
as defined by the United States Pharmacopoeia (USP DIVolume III: Approved Drug
Products and Legal Requirements). (see “Compound Prescriptions” section)
• Oral contraceptives (plan specific)
• Blood glucose test strips
• Flu vaccine
Covered Injectable and Specialty Medications
Most Select Health plans have specialty benefits incorporated in the benefit structure.
This allows pharmacies to bill covered injectable drugs and specialty medications
through the pharmacy benefit. Some injectable drugs may be covered under other
tiers of the pharmacy benefit when not classified as a specialty injectable medication
according to Select Health formularies.
For questions on coverage of specific injectable and specialty medications, the
pharmacy may contact the Select Health Pharmacy Help Desk for assistance.
Generally Excluded Medications and Services
Most prescription drugs for covered medical conditions are covered by the prescription
drug benefit. However, unless noted otherwise in plan documents or preauthorized as
an exception by the plan, the following drugs are not covered under the prescription
drug benefit but may be covered elsewhere under the medical benefit:
• Certain drugs with a therapeutic over-the-counter (OTC) equivalent
• Drugs purchased from Out-of-Network Providers over the Internet
• Flu symptom drugs, except when approved by an expert panel of Physicians and
Select Health
• Non-Sedating Antihistamines
• Prescription drugs used to inhibit and/or suppress drowsiness, sleepiness, tiredness,
or exhaustion
• Replacement of lost, stolen, or damaged drugs
• Sexual dysfunction drugs

17
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
• Travel-related medications, including preventive medication for the purpose of travel
to other countries
• All non-prescription contraceptive jellies, ointments, foams, and/or devices, such as
IUDs
• Appetite suppressants and weight loss medications
• Certain off-label drug usage, unless the use has been approved by a Select Health
Medical Director or clinical pharmacist
• Compound drugs when alternative products are available commercially
• Cosmetic agents, health or beauty aids, or prescriptions used for cosmetic purposes,
including minoxidil for hair growth
• DMSO (dimethyl sulfoxide)
• Drugs not meeting the minimum levels of evidence based upon Food and Drug
Administration (FDA) approval, the drug has no active ingredient and/or clinically
relevant studies as determined by Select Health
• Drugs or medicines purchased and received prior to the member’s effective date of
coverage or after the member’s termination of coverage
• Food supplements, food substitutes, medical foods, and formulas
• Human growth hormone
• Infertility medications or drugs used for infertility purposes
• Medication not requiring a prescription, even if ordered by a participating provider by
means of a prescription, and drugs that are not medically necessary or that are used
inappropriately
• Medication which may be properly received without charge under local, state,
or federal programs or which are reimbursable under other insurance, including
Worker’s Compensation
• Pharmacy & Therapeutics Committee, nationally recognized compendium sources
currently utilized by Select Health, National Comprehensive Cancer Network (NCCN),
or as defined within Select Health’s Preauthorization criteria or medical policy
• Minerals, fluoride, and vitamins other than prenatal or when determined to be
Medically Necessary to treat a specifically diagnosed disease
• Non-prescription vitamins
• Over-the-counter (OTC) medications, except when all of the following conditions
are met:
— The OTC medication is listed on the Select Health formulary as a covered medication.
— The Select Health Pharmacy & Therapeutics Committee has approved the OTC
medication as a medically appropriate substitution of a prescription drug or
medication.
— The member has obtained a prescription for the OTC medication from a licensed
provider and filled the prescription at a participating pharmacy.

18
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
• Prescriptions written by a licensed dentist, unless for the prevention of infection or
pain in conjunction with a dental procedure.
• Progesterone powder (micronized progesterone), except when prior authorized
during pregnancy or other FDA-approved use.
• Therapeutic devices or appliances including hypodermic needles, syringes, support
garments, and other non-medicinal substances (except insulin syringes, glucose test
strips, and inhaler extensions).
Covered Medications and Services
The Select Health formulary for the Medicare Advantage plan has five tiers with
coverage of most Part D generic drugs and most Part D brand drugs.
Any injectable medication considered part of the Medicare Part D benefit will be
eligible for processing under the member’s pharmacy benefit, even if the service is
submitted under the medical benefit.
Generally Excluded Part D Medications
Non-Part D drugs, including prescription drugs covered by Part A or Part B and other
drugs excluded from coverage by Medicare.
Diabetic Supplies
Lancets and Test Strips, through part of the Medicare Part B benefit, will be allowed to
process at the pharmacy through the POS.
Step Therapy
Select Health Medicare requires Step Therapy for certain drugs. This means that
certain drugs are covered by the Medicare plan only after the member has tried the
alternative therapy without success.
Exceptions and Coverage Determinations
At any time, a member may request a coverage determination or an exception to a
prior authorization requirement or other edit imposed by the Medicare Part D plan.
The individual member, member’s representative, or the prescribing physician or
other prescriber may initiate the exception request. Common reasons for requesting
coverage determination or an exception are:
• For coverage of a drug that requires prior authorization
• For coverage of a drug that is not covered on the plan’s formulary
• To bypass step therapy or quantity limit restrictions
• To cover a drug at a lower tier
7.2 SELECT HEALTH
MEDICARE
MEDICARE
PART D

19
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
If an exception is approved, it will generally be honored for the remainder of the plan
year with no requirement to initiate another coverage determination each time the
medication is being filled.
There is no guarantee that a request for exception will be granted. Each request will be
evaluated individually based on the situation at hand.
Part B and Part D Benefit Overlap
Drugs that are eligible under a member’s Medicare Part B benefit are not eligible
for coverage under the Part D benefit. The determination for under which benefit a
drug will be covered is not just determined by the drug itself, but also its indication
and administration. Medicare Part B covers a limited list of specific drugs including
injectable and infusible drugs that are not usually self-administered. Edits will be
applied in the Select Health system to manage these rules at adjudication.
Exceptions to Plan Coverage
Exceptions to Select Health Medicare Plan coverage include any pharmacy claims
processed from a foreign pharmacy. Claims processed at pharmacies outside the
United States will not be paid through the Select Health Medicare Advantage program.
The Select Health Community Care plan generally covers all medications included on
the Prescription Drug Formulary for Traditional and Non-Traditional enrollees.
There are some drugs that will continue to be covered by the State Medicaid agency.
Coverage and applicable costs are not decided by Select Health Community Care.
Therapeutic classes carved out include:
• Attention deficit hyperactivity disorder (ADHD)
• Antidepressant
• Anti-anxiety
• Anticonvulsant
• Antipsychotic
• Hemophilia factor
• Immunosuppressive
• Substance abuse (opioid or alcohol)
Medical necessity is evaluated for services typically not covered for children and
pregnant women.
7.3 SELECT HEALTH
COMMUNITY CARE
MEDICAID

20
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
General exclusions include these services:
• Duplicate prescription for lost, stolen, destroyed, spilled, or otherwise non-usable
medication with some exceptions
• Compounded prescriptions
• Lozenges, suckers, rapid dissolve, lollipop, pellets, patches, or
other unique formulation delivery methodologies developed to garner “uniqueness,”
except where the specific medication is unavailable in any other form
• Specific excluded drug classes:
— Cosmetic preparations
— Minerals
— Patches
— Weight gain or loss
— Vitamins, except when provided for:
• Pregnant women: prenatal vitamins with folic acid (prenatal vitamins are not
covered post-delivery)
• Children through age five: children’s vitamin drops with or without fluoride
• Adults and children of all ages: fluoride supplement
• Covered outpatient drugs that the manufacturer seeks to require as a condition of
sale for which associated tests and monitoring services are purchased exclusively
from the manufacturer or its designee
• Agents used for the treatment of sexual or erectile dysfunction

21
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
8.0 Common Reject Messages
Message Explanation
09: M/I
Birth Date
Select Health requires a valid date of birth for the cardholder ID to be submitted in order to verify
eligibility and process claims. If the member’s date of birth is submitted incorrectly, the pharmacy will
receive the M/I Birth Date rejection. When received, the pharmacy should contact the Select Health
Help Desk to verify the correct information and for assistance in processing.
13: M/I Other
Coverage Code
The M/I Other Coverage Code error message may appear when a claim is being submitted to Select
Health as the secondary payer and Select Health does not have record of other health insurance for
the member. When received, the pharmacy should contact the Select Health Help Desk to verify the
correct order of benefits information and for assistance in processing.
40: Pharmacy
Not Contracted
with Plan on
Date of Service
Select Health requires an active contract for pharmacies to submit claims for payment at point of
sale. When the Pharmacy Not Contracted with Plan on Date of Service error is received, the pharmacy
should contact the Select Health Help Desk to verify their contract status.
41: Submit
Bill to Other
Processor or
Primary Payor
The Submit Bill to Other Processor or Primary Payor error message may appear when a claim is
being submitted to Select Health as the primary payer and Select Health records have other health
insurance on file as the primary payor for the member. When received, the pharmacy should contact
the Select Health Help Desk to verify the correct order of benefits information and for assistance in
processing.
52: Non-
Matched
Cardholder ID
Select Health requires a valid cardholder ID to be submitted in order to verify eligibility and process
claims. The ID number is the 9-digit subscriber ID number that can be found on the member’s ID card.
If the member’s ID number or the member’s date of birth is submitted incorrectly, the pharmacy will
receive the Non-Matched Cardholder ID rejection. When received, the pharmacy should contact the
Select Health Help Desk to verify the correct information and for assistance in processing.
70: Product/
Service Not
Covered and
MR: Product
Not on
Formulary
This error message may appear for a member with a formulary requirement. If this is the case, the
online system will not return financial information and the prescription will not be reimbursed by Select
Health.
Select Health members have the following options should this rejection be received:
• Consult with the prescribing physician to discuss formulary alternatives prior to having the pre-
scription filled
• Pay in full for the non-covered medication and discuss formulary alternatives for future fills (this is
not reimbursable)
• Pay in full for the non-covered medication
Contact the Select Health Member Services line for assistance in determining prescription benefit
coverage. Pharmacists may also contact the member’s prescribing physician to discuss formulary
alternatives and/or formulary exception requests, which can be initiated by the prescribing physician.
Please note that if the member pays in full for the non-covered medication, Select Health does not
guarantee that reimbursement will be made, either retroactively or for future fills.

22
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Message Explanation
71: Prescriber
is Not Covered
There are several situations that could cause a Prescriber is Not Covered error. Below are the most
common examples:
• Select Health requires a valid NPI number for prescriber identification. Select Health relies on the
pharmacy for submission of accurate information.
• Some plans require that the prescribing physician participate in the Select Health physician net-
work for a medication to be covered.
• The prescriber may be sanctioned by the Office of Inspector General (OIG).
75: Prior
Authorization
Required
There are certain medications that Select Health requires prior authorization before the medication
can be dispensed to the member. When this rejection is received, the pharmacy may contact the Se-
lect Health Help Desk to begin the prior authorization process. The Select Health Prescription Drug List
(PDL) notates the medications that require prior authorization with a “(PA)” in the “Spec. Requirements”
column. For the most up-to-date drug information, access the PDL through the Select Health website.
76: Plan
Limitations
Exceeded
The Plan Limitations Exceeded rejection could occur for a variety of reasons, including the
most common:
• Over Quantity Limits:
— This could be caused by a dose optimization issue which would require the prescribing physician’s
office to change to a different strength of the same medication.
— Alternatively, the prescribing physician can send into Select Health a Letter of Medical Necessity
(LMN) for review as originally prescribed.
— As a final option, the pharmacy can resubmit the prescription for the amount Select Health will allow.
• Cost Exceeds Maximum:
— Select Health applies a max cost per prescription of $1,000; in most instances when this reject is
received for exceeding the max cost edit, the pharmacy can call the Select Health Help Desk for an
override.
— Compound medications have a different cost edit of $75 per prescription; in many cases, a compound
medication will require a LMN from the prescribing physician to obtain the necessary cost override.
— Over Day Supply Limits: Select Health applies a max day supply that can vary by plan and by drug. If
the pharmacy has questions if this rejection is received, please contact the Pharmacy Help Desk for
assistance.
— Patient Age Exceeds Maximum Age Allowed for Drug: Select Health applies age limitations to
applicable medications depending on safety, efficacy, or specialized dosage form.
— Over Maximum Daily Dose: Select Health may apply a maximum daily dose based on the U.S. Food
and Drug Administration (FDA) approved labeling and other accepted drug compendia guidelines
meeting minimum levels of evidence.
79: Refill Too
Soon
Select Health applies an edit for refilled medications that require the medication be 75% gone before a
refill can be allowed, for most plans. For controlled substances the edit requires that the medication be
80% gone before a refill can be allowed. Contact the Select Health Pharmacy Help Desk for additional
information or assistance processing.

23
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Message Explanation
88: DUR Reject
Error
There are several situations that could cause a DUR Reject Error. The most common examples are:
• Opioid Care Coordination: Select Health will give a soft rejection when prescriptions are written
for more than 90 morphine milligram equivalents (MME) daily. For a Medicare or commercial
member, the pharmacist must verify dosing and plan with the prescriber. After verification has
taken place, the pharmacy can override the edit using a Submission Clarification Code of 07:
Medically Necessary. For a Medicaid member the maximum restriction is 90 morphine milligram
equivalents (MME) daily and cannot be overridden on the pharmacy side.
• Opioid High-Dosage Limits: Select Health will reject claims when filling for a high-dose opioid,
greater than 200 MME for most plans. For Medicaid members, Select Health will reject claims
when filling for a high-dose opioid, greater than 90 MME. The patient or prescriber is required to
send a prior authorization request to Select Health if they believe an exception should be granted
for this restriction.
• Seven-Day Max Fill For Opioid Naïve Patients: Select Health will only allow a maximum 7-day fill
for any patient that is opioid naïve for their first fill. (For a Medicaid member, opioids prescribed by
a dentist are limited to a maximum 3-day fill.)
• Concurrent Benzodiazepine and Opioid Therapy: Select Health will give a soft rejection when a
patient has overlapping days supplies of benzodiazepine and opioid medications. The pharmacist
must verify dosing and plan with the prescriber. After verification has taken place, the pharmacy
can override the edit using a submission clarification code of 07: Medically Necessary.
• Multiple Long-Acting Opioid Prescriptions: Select Health will give a soft rejection when a patient
attempts to fill more than one long-acting opioid medication with overlapping days supplies. The
pharmacist must verify dosing and plan with the prescriber. After verification has taken place, the
pharmacy can override the edit using a submission clarification code of 07: Medically Necessary.
569: Provide
Notice:
Medicare
Prescription
Drug Coverage
and Your
Rights
When a claim for a Medicare Part D drug is submitted to the Select Health Medicare plan and is not
covered on the formulary or exceeds formulary limitations and is outside the Medicare Part D tran-
sition fill coverage period, the Provide Notice: Medicare Prescription Drug Coverage and Your Rights
rejection will be sent. When this rejection is received and the member must leave the pharmacy
without their prescription, the pharmacy is required to provide the member with the Member’s Rights
document.
608: Step
Therapy,
Alternate
Drug Therapy
Required
Prior To Use
of Submitted
Product
Service ID
Select Health applies Step Therapy edits to certain medications, which will require qualifying medica-
tion(s) before Select Health will cover the one that is rejecting. If those step therapy rules have not been
met, the pharmacy will receive this rejection.

24
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
9.0 Payment and Reconciliation Information
9.1 PAYMENT
SCHEDULE
Select Health Commercial, Scripius PBM Products, and Select Health
Community Care (Utah State Medicaid)
For reimbursement to the pharmacies, payment cycles are run every two (2) weeks.
Checks will be disbursed within fifteen (15) working days of the end of the cycle and
will be mailed to the pharmacy.
Select Health Medicare (Medicare Part D)
For reimbursement to the pharmacies for Medicare claims, Select Health will
issue, mail, or otherwise transmit payment for all clean claims, submitted by
network pharmacies (other than mail-order and long-term care pharmacies) within
fourteen(14) days after the date the claim is received for an electronic claim or
thirty(30) days after the date the claim is received for any other claim.
Each payment to the pharmacy will be accompanied by one copy of the Pharmacy
Claims Reconciliation Report. This report will provide a detailed list of all claims
submitted during the current cycle for each pharmacy and will provide totals for the
reconciliation or the payment amount. This report will include all paid, rejected, and
reversed claims for the current processing cycle. As an alternative format, the report
can also be made available in 835 format, delivered via sFTP in place of the paper
remittance report.
Additional copies of the Claims Reconciliation Summary Report may be obtained
by request from the Select Health Pharmacy Help Desk. There will be a charge
per additional copy requested. Questions regarding the payment cycle and
remittance files should be directed to the Select Health Pharmacy Networks Team at
SHPharmacyContr[email protected]g.
Pharmacies wishing to receive payments via Electronic Funds Transfer (EFT) may
submit a request to the Select Health Pharmacy Networks Team by emailing
Please note that pharmacies must receive their Remittance Report via 835 file format.
No paper Remittance Report would be supplied to the pharmacy.
Federal requirements dictate that a rebate or discount is required for all covered
outpatient drugs for Medicaid plans. Select Health will collect all forfeited rebate
amounts resulting from 340B Claims.
9.2 REMITTANCE
REPORT
9.3 ELECTRONIC
FUNDS TRANSFER
EFT
9.4 340B CLAIMS

25
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
10.0 Select Health Medicare (Medicare Part D): Specific Information
10.1 PLAN SUMMARY
Select Health’s Medicare plan is an MAPD plan that covers parts of Utah, Idaho,
and Nevada. The plan is committed to following Centers for Medicare and Medicaid
Services (CMS) guidelines and ensuring access to necessary medications while
working closely with the pharmacies to provide the best customer experience possible.
It is expected that the provider agrees to adhere to the CMS Prescription Drug Benefit
Manual, Chapter 9 Part D Program to Control Fraud, Waste, and Abuse, and Part
D Sponsors’ policies and procedures, training and corrective action plans related to
the program. Cooperation with the Part D Plan Sponsor includes providing copies
of prescriptions, signature logs, and other related documentation to assist in any
investigations.
To be considered a pharmacy in compliance with Medicare Part D rules and
regulations, pharmacies must agree under CMS guidelines to provide ongoing
Medicare Part D training and documentation to its staff.
As part of the audit process with Select Health, copies of this training and record of the
staff receiving the training may be required to be produced, as needed.
To process Medicare Part D claims for Select Health, pharmacies are required to sign a
specific Medicare contract addendum. If not signed, any Medicare claims processed to
Select Health will be rejected at POS.
Veterans’ Administration benefits are separate and distinct from benefits provided
under Medicare Part D, per federal regulations. By law, VA cannot bill Medicare. A
beneficiary may not use both VA prescription drug benefits and Part D benefits for a
single prescription.
To be in compliance with CMS requirements, if a member should present a Part D
acknowledgment letter in place of an ID card, the pharmacy should honor that letter
as sufficient eligibility to process a claim to Select Health for their Medicare Part D
benefit. If the presented letter does not contain sufficient information to process a
claim to Select Health, please contact the Select Health Medicare Part D Help Desk for
assistance in processing.
In accordance to the transition plan requirements from CMS, Select Health will offer
short-term coverage for Part D benefits to members that are new to the plan. During
this transition period, a member can receive an initial fill of an ongoing medication
even if it is not covered under the new Medicare Part D plan (including if it requires
prior authorization or step therapy). It is assumed that during this transition period,
10.2 FRAUD, WASTE,
AND ABUSE
10.3 TRAINING
10.4 PHARMACY
CERTIFICATION
FOR PART D
10.5 FEDERAL HEALTH
CARE PROGRAMS
PARTICIPATION
EXCLUSION
10.6 GENERAL
PROCEDURES FOR
ACKNOWLEDG
MENT LETTERS
10.7 FORMULARY
TRANSITION
FILL PLAN

26
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
the member will be working with their physician to identify alternative equivalent
medications that are covered under the plan.
For long-term care facilities to process Medicare Part D claims to Select Health, the
pharmacy is required to sign a specific LTC Medicare contract addendum. If not signed,
any Medicare claims processed to Select Health will be rejected at POS.
For a home infusion pharmacy to process Medicare Part D claims to Select Health,
the pharmacy must sign a specific home infusion Medicare contract addendum. If not
signed, any Medicare claims processed to Select Health will be rejected at POS.
The Select Health Medicare Advantage program covers the following service areas:
• Utah Counties: Box Elder, Cache, Davis, Franklin (ID), Garfield, Iron, Juab, Millard,
Morgan, Piute, Rich, Salt Lake, Sanpete, Sevier, Summit, Tooele, Utah, Washington,
Wayne, Weber
• Idaho Counties: Ada, Adams, Boise, Canyon, Cassia, Elmore, Gem, Gooding, Jerome,
Minidoka, Owyhee, Payette, Valley, Twin Falls, Washington
• Nevada Counties: Clark, Nye
• Colorado Counties: Adams, Arapahoe, Broomfield, Boulder, Clear Creek, Delta,
Denver, Douglas, Elbert, El Paso, Gilpin, Jefferson, Mesa, Park, Pueblo, Teller
10.8 LONGTERM
CARE LTC
FACILITIES
10.9 HOME INFUSION
THERAPY
10.10 MEDICARE
SERVICE AREA

27
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
11.0 Select Health Community Care (Medicaid): Specific Information
Pharmacies that contract to provide services to Select Health Community Care
members must also be a participating provider with Utah Medicaid. See the Utah
State Medicaid Provider Manual for more information.
All written prescriptions for drugs under the Medicaid program must be on tamper-
resistant prescription pads.
Compliance with all federal and state laws regarding the types of documentation and
how prescriptions are filled must be maintained.
To be considered “tamper resistant,” Medicaid written prescriptions must contain one
or more industry-recognized features designed to prevent:
1. Unauthorized copying of a completed or blank prescription form;
2. The erasure or modification of information written on the prescription by the
prescriber; and
3. The use of counterfeit prescription forms.
Medicaid requires use of generic drugs, unless the physician obtains a prior approval
for the brand name drug. However, Medicaid does not pay for generic house-brand or
store-brand products unless the manufacturer has entered into a rebate agreement
for each specific NDC number. Manufacturers that have not entered the federal rebate
program will not have their products covered. This includes almost all ‘house-brand’
and ‘store-brand’ products.
Some medications that require preauthorization may be provided in a medical
emergency before authorization is obtained from Select Health. When a medical
emergency occurs, and a medication requiring a preauthorization is required,
pharmacy providers may provide up to a 72-hour supply of the medication. When
contacted, Medicaid will issue an authorization for the 72-hour supply of the medication
on the next business day. All subsequent quantities must meet all plan requirements
for the medication. It is the responsibility of the medication prescriber to provide the
necessary documentation.
Select Health Community Care enrollees who inappropriately utilize health care
services may be enrolled in the Restriction Program. Enrollees are identified for
enrollment through:
• Periodic review of patient profiles to identify inappropriate over-utilization of medical
providers, urgent care centers, specialists, medications, and/or pharmacies.
• Verbal and written reports of inappropriate use of services generated by one or more
health care providers regarding the member. These reports are verified through a
review of the patient’s claim history by Medicaid staff and medical consultants.
• Referral from Medicaid staff.
11.1 TAMPER
RESISTANT
PRESCRIPTION PAD
REQUIREMENTS
11.2 GENERIC
PREPARATIONS
11.3 MEDICATIONS
PROVIDED IN A
MEDICAL
EMERGENCY
11.4 RESTRICTION
PROGRAM

28
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Enrollees in the Restriction Program are informed of the reasons for enrollment,
counseled in the appropriate use of health care services, and assigned a Primary
Care Provider and a pharmacy. In addition to the Select Health Community Care
card, enrollees will receive a Utah Medicaid card, which identifies the enrollee as
“RESTRICTED” below the eligibility information and above the member’s name. These
clients must receive all health care services through either the assigned primary
care provider or receive a referral from this primary care to see any other provider. All
pharmacy services must be received from the assigned pharmacy. Select Health will
only pay claims for services rendered by providers:
• Listed on the card; and
• From whom members were appropriately referred.
Emergency services are not restricted to assigned providers.

29
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
Appendix: Payer Sheet
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 1 of 13
General Information
Payer Name: SelectHealth, Inc.
Date: 5/1/2024
Plan Name/Group Name:
BIN:
PCN:
GROUP:
Select Health Commercial
8ØØØØ8
Not required
Not required
Scripius (PBM)
8ØØØØ8
Not required
Not required
Select Health Medicaid
8ØØØØ8
6Ø6
Not required
Select Health Medicare
Ø15938
7463
Printed on card
Select Health Worker’s Compensation
Ø183Ø8
WCØØ1
Not required
Intermountain Rx Charity Program
Ø24Ø61
PA123
Not required
Avera Health
Ø26952
AVERA
Not required
Effective as of: 9/21/2020
NCPDP Telecommunication Standard
Version/Release: DØ
ECL version: July 2Ø14
Certification Testing Window: N/A
Certification Contact Information: Rx_BA@imail.org
Provider Relations Contact Information: [email protected]
Other Contact Information:
Select Health Pharmacy Services 8ØØ-442-3129
M-F 7:ØØ AM – 9:ØØ PM (MST) Sat 9:ØØ AM – 3:ØØ PM (MST)
Select Health Medicare Pharmacy Services 855-442-9988
Medicare Assistance Available 24 hours a day / 7 days a week
Maximum Number of Transactions
Supported Per Transmission
1 – Medicare
4 – Commercial/Medicaid
Submission and Reversal Window (days
from date filled/dispensed to date
submitted)
Commercial
9Ø Days
Medicaid
9Ø Days
Medicare
9Ø Days
If an exception is needed, please contact
SelectHealth Pharmacy Services
Supported Transactions

30
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials
reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated
January 1, 2024 Page 2 of 13
Transaction
Code
Transaction Type
B1, B3
Billing
B2
Reversal
E1
Eligibility Inquiry

31
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 3 of 13
Table Legend
Payer Usage
Value
Explanation
Payer
Situation
Mandatory
M
Mandatory for the segment in the designated transaction in
accordance with NCPDP Telecommunication Implementation
Guide, Version DØ.
No
Required
R
Required as defined by the processor.
No
Qualified
Requirement
RW
Required as defined by the situation.
Yes
Segment and Field Requirements
The following lists the segments and fields in a Billing transaction based on the NCPDP
Telecommunication Standard Implementation Guide Version DØ.
Fields that are not used in the Claim Billing/Claim Rebill transaction, and those that do not have
qualified requirements (e.g. not used) for this payer, are excluded.
Claim Billing/Claim Rebill Transaction
Transaction Header Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
1Ø1-A1
BIN Number
M
8ØØØØ8 – Commercial/Medicaid/PBM
Ø15938 – Medicare
Ø183Ø8 – Workers’ Compensation
Ø24Ø61 – Intermountain Rx Charity Program
Ø26952 – Avera Health
1Ø2-A2
Version/Release Number
M
DØ
1Ø3-A3
Transaction Code
M
B1, B3
1Ø4-A4
Processor Control
Number
M
6Ø6 – Medicaid
7463 – Medicare
PA123 – Intermountain Rx Charity Program
AVERA- Avera Health
1Ø9-A9
Transaction Count
M
Ø1 – 1 occurrence (Required for Medicare)
Ø2 – 2 occurrences
Ø3 – 3 occurrences
Ø4 – 4 occurrences
2Ø2-B2
Service Provider ID
Qualifier
M
Ø1 – NPI

32
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 4 of 13
2Ø1-B1
Service Provider ID
M
1Ø digit NPI number
4Ø1-D1
Date of Service
M
CCYYMMDD
11Ø-AK
Software
Vender/Certification ID
M
Use value for Switch’s requirements or send
spaces
Insurance Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø4 – Insurance Segment
3Ø2-C2
Cardholder ID
M
9-character ID beginning with 8Ø.
312-CC
Cardholder First Name
R
313-CD
Cardholder Last Name
R
3Ø3-C3
Person Code
R
Not required unless patient is a twin, triplet, etc.,
covered under the same policy or if otherwise
instructed by Pharmacy Services
3Ø6-C6
Patient Relationship Code
R
36Ø-2B
Medicaid Indicator
RW
Submit when patient has Medicaid coverage
115-N5
Medicaid ID Number
RW
Required if known, when patient has Medicaid
coverage
3Ø1-C1
Group ID
RW
Required for all Medicare Part D claims:
U1ØØØØØ9
U1ØØØØ11
Required only if printed on card or otherwise
communicated by SelectHealth for Workers’
Compensation claims.
Patient Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø1 – Patient Segment
331-CX
Patient ID Qualifier
M
Ø4 – Health Plan Assigned
332-CY
Patient ID
M
3Ø4-C4
Date of Birth
R
3Ø5-C5
Patient Gender Code
R
1 – Male
2 – Female
31Ø-CA
Patient First Name
R
311-CB
Patient Last Name
R
384-4X
Patient Residence
RW
Required for all Medicare Part D claims:

33
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 5 of 13
Ø – Not Specified
1 – Home
2 –
Skilled Nursing Facility (Part B only with prior
authorization)
3 – Nursing Facility (required for Part D Short-
Cycle Dispensing claims)
4 – Assisted Living Facility
5 – Custodial Care Facility (Part B only with prior
authorization)
6 – Group Home
9 – Intermediate Care Facility/Mentally Retarded
11 – Hospice
3Ø7-C7
Place of Service
RW
Required for all Medicare Part D claims
Claim Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
This payer does not support partial
fills
X
Pharmacies should reverse and reprocess initial
claim when they have satisfied the requirements
as written on the prescription
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø7 – Claim Segment
455-EM
Prescription/Service
Reference Number
Qualifier
M
1 – Rx Billing
4Ø2-D2
Prescription/Service
Reference Number
M
436-E1
Product/Service ID
Qualifier
M
Ø3 – National Drug Code (NDC)
4Ø7-D7
Product/Service ID
M
NDC
442-E7
Quantity Dispensed
R
4Ø3-D3
Fill Number
R
Ø – Original Dispensing
1-99 – Refill Number
4Ø5-D5
Days Supply
R
4Ø6-D6
Compound Code
R
1 – Not a Compound
2 – Compound
4Ø8-D8
Dispense As Written
(DAW)/Product Selection
Code
R
414-DE
Date Prescription Written
R
CCYYMMDD
415-DF
Number of Refills
Authorized
R
419-DJ
Prescription Origin Code
R
1 – Written
2 – Telephone

34
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 6 of 13
3 – Electronic (excludes fax, e-mail, internal clinic
messaging system or a physician printing to a
printer at the pharmacy)
4 – Facsimile (fax)
5 – Pharmacy
42Ø-DK
Submission Clarification
Code
RW
Required for Medicaid 34ØB claims:
2Ø – 34ØB
Required for Medicare Part D claims when
Patient
Residence = 3:
16 – LTC Emergency Box (Kit) or Automated
Dispensing Machine
22 – LTC Dispensing: 7 days
23 – LTC Dispensing: 4 days
24 – LTC Dispensing: 3 days
25 – LTC Dispensing: 2 days
26 – LTC Dispensing: 1 day
27 – LTC Dispensing: 4-3 days
28 – LTC Dispensing: 2-2-3 days
29 – LTC Dispensing: Daily and 3-day weekend
3Ø – LTC Dispensing: Per shift dispensing
31 – LTC Dispensing: Per med pass dispensing
32 – LTC Dispensing: PRN on demand
33 – LTC Dispensing: 7 day or less cycle not
otherwise represented
34 – LTC Dispensing: 14 days
35 – LTC Dispensing: 8-14 day dispensing
method not listed above
3Ø8-C8
Other Coverage Code
RW
1 – No Other Coverage
2 – Other Coverage Exists – Payment Collected
3 – Other Coverage Billed – Claim Not Covered
4 – Other Coverage Exists – Payment Not
Collected
453-EJ
Originally Prescribed
Product/Service ID
Qualifier
RW
Required when medication was changed from the
original script
445-EA
Originally Prescribed
Product/Service Code
RW
Required if submitting a claim that replaces an
originally prescribed product/service
446-EB
Originally Prescribed
Quantity
RW
Required if submitting a claim that replaces an
originally prescribed product/service
147-U7
Pharmacy Service Type
RW
Required for all Medicare Part D claims
429-DT
Special Packaging
Indicator
RW
Required for Medicare Part D claims when Patient
Residence Code = 3
46Ø-ET
Quantity Prescribed
RW
Required for all Schedule II drugs

35
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 7 of 13
Pricing Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
11 – Pricing Segment
4Ø9-D9
Ingredient Cost Submitted
R
412-DC
Dispensing Fee Submitted
R
481-HA
Flat Sales Tax Amount
Submitted
RW
Required when provider is claiming sales tax and
its value has an effect on the Gross Amount Due
(43Ø-DU) calculation
482-GE
Percentage Sales Tax
Amount Submitted
RW
Required when provider is claiming sales tax and
its value has an effect on the Gross Amount Due
(43Ø-DU) calculation
483-HE
Percentage Sales Tax Rate
Submitted
RW
Required if needed to calculate Percentage Sales
Tax Amount Paid (559-AX)
484-JE
Percentage Sales Tax Basis
Submitted
RW
Required if needed to calculate Percentage Sales
Tax Amount Paid (559-AX)
426-DQ
Usual and Customary
Charge
M
43Ø-DU
Gross Amount Due
R
423-DN
Basis of Cost
Determination
R
Ø1 – AWP
Ø7 – U&C
1Ø – ASP
12 – WAC
Pharmacy Provider Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø2 – Pharmacy Provider Segment
465-EY
Provider ID Qualifier
R
444-E9
Provider ID
R
Prescriber Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø3 – Prescriber Segment
466-EZ
Prescriber ID Qualifier
R
Ø1 – NPI (Required for Medicare)
12 – DEA
411-DB
Prescriber ID
R
427-DR
Prescriber Last Name
R

36
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 8 of 13
Coordination of Benefits/Other
Payments Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is situational
X
Required only for secondary, tertiary, etc. claims
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø5 – Coordination of Benefits/Other Payments
Segment
337-4C
Coordination of
Benefits/Other Payments
Count
M
Maximum count of 9
338-5C
Other Payer Coverage
Type
M
Ø1 – Primary
Ø2 – Secondary
Ø3 – Tertiary
339-6C
Other Payer ID Qualifier
R
Ø3 – BIN
34Ø-7C
Other Payer ID
R
BIN
443-E8
Other Payer Date
R
341-HB
Other Payer Amount Paid
Count
RW
Required when Other Payer Amount Paid (431-
DV) is specified
Maximum count of 9
Value should be greater than zero when OCC = 2
or 4; blank/null when OCC = 3
342-HC
Other Payer Amount Paid
Qualifier
RW
Required when Other Payer Amount Paid (431-
DV) is specified
431-DV
Other Payer Amount Paid
RW
Required when Other Payer Amount Paid Count
(341-HB) is specified
Value of the sum of all payers should be greater
than zero when OCC = 2; zero when OCC = 4;
blank/null when OCC = 3
471-5E
Other Payer Reject Count
RW
Required when claim has been rejected by previous
payer(s) and the Other Payer Reject Code (472-
6E)
is specified
Maximum count of 5
Value should be blank/null when OCC = 2 or 4;
greater than zero when OCC = 3
472-6E
Other Payer Reject Code
RW
Required when Other Payer Reject Count (471-5E)
is specified and Other Coverage Code (3Ø8-C8) =
3
Value should be other payer NCPDP Reject Code
353-NR
Other Payer-Patient
Responsibility Amount
Count
RW
Required when Other Payer-Patient Responsibility
Amount (352-NQ) is specified

37
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 9 of 13
Maximum count of 25
Allowed if OCC = 2 or 4; not allowed if OCC = 3
351-NP
Other Payer-Patient
Responsibility Amount
Qualifier
RW
Required when Other Payer-Patient Responsibility
Amount (352-NQ) is specified
Components of Patient Pay are required for values
Ø1 – Ø5 and Ø7 – 13
Usage of Ø6 “Patient Pay as Reported by Previous
Payer” accepted as an exception and subject to
audit
352-NQ
Other Payer-Patient
Responsibility Amount
RW
Required when Other Payer-Patient Responsibility
Amount Count (353-NR) is specified and when
necessary for state/federal/regulatory agency
programs
Must be submitted for accurate pricing calculations
on OCC 2 and 4, for all SelectHealth Commercial
The COB segment and all required fields must be sent if the Other Coverage Code (3Ø8-C8) = 2, 3, or 4.
Note: When Other Coverage Code (3Ø8-C8) = 2 (Other Coverage Exists – payment collected), fields 341-HB,
342-HC and 431-DV are required.
Compound Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is situational
X
Only required for submission of a compound
claim (Field 4Ø6-D6 = 2)
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
1Ø – Compound Segment
45Ø-EF
Compound Dosage Form
Description Code
M
Ø1 – Capsule
Ø2 – Ointment
Ø3 – Cream
Ø4 – Suppository
Ø5 – Powder
Ø6 – Emulsion
Ø7 – Liquid
1Ø – Tablet
11 – Solution
12 – Suspension
13 – Lotion
14 – Shampoo
15 – Elixir
16 – Syrup
17 – Lozenge
18 – Enema
451-EG
Compound Dispensing
Unit Form Indicator
M
1 – Each
2 – Grams
3 – Milliliters
447-EC
Compound Ingredient
Component Count
M
Count must match the submitted number of
repetitions
Maximum 25 ingredients
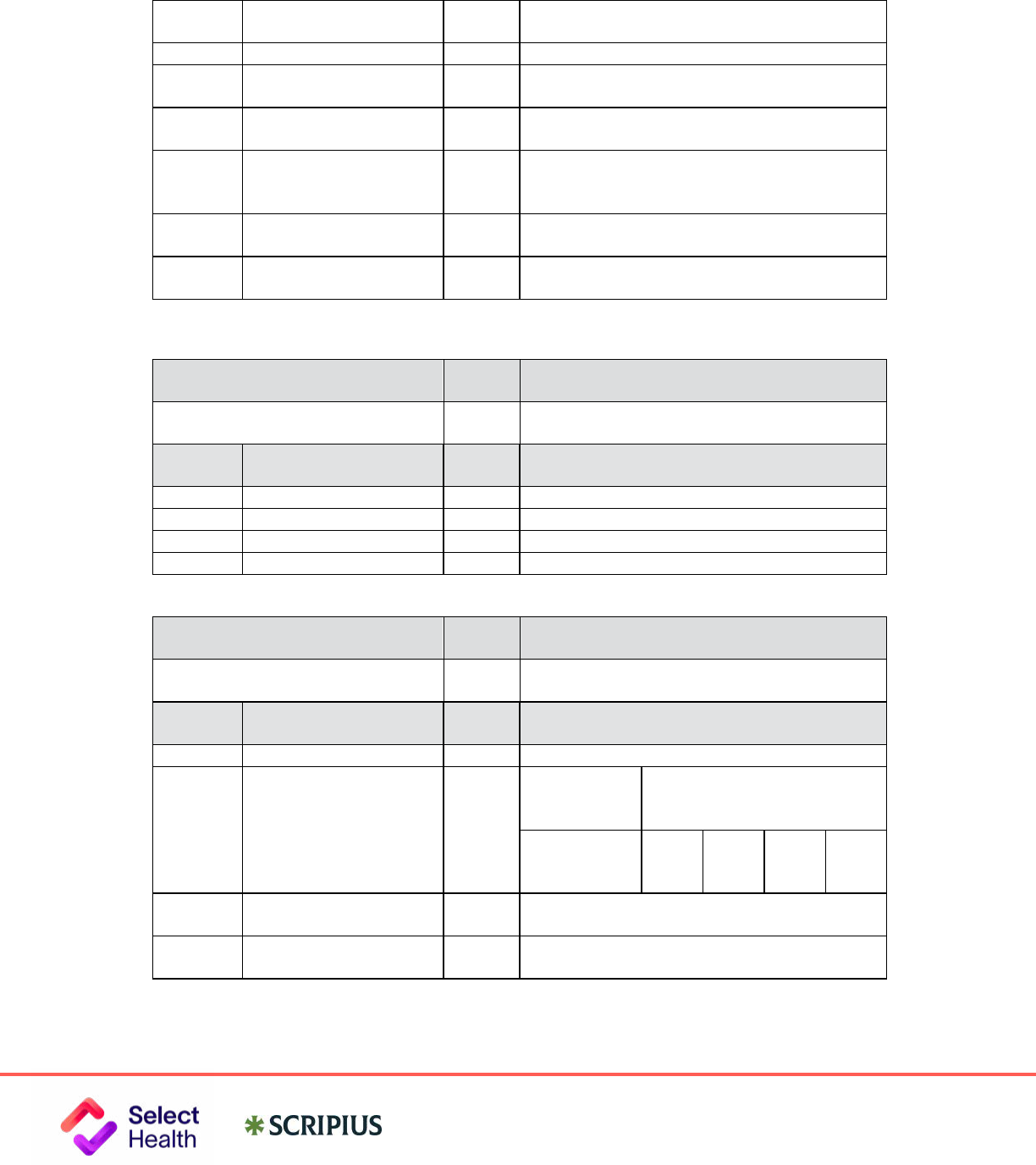
38
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 10 of 13
488-RE
Compound Product ID
Qualifier
M
Ø3 - NDC
489-TE
Compound Product ID
M
Component NDC(s) of compound
448-ED
Compound Ingredient
Quantity
M
Amount expressed in metric decimal units
449-EE
Compound Ingredient
Drug Cost
R
49Ø-UE
Compound Ingredient
Basis Of Cost
Determination
R
362-2G
Compound Ingredient
Modifier Code Count
R
Maximum count of 1Ø
363-2H
Compound Ingredient
Modifier Code
R
Note: The sum of all Compound Ingredient Drug Costs (449-EE) must equal Ingredient Cost
Submitted (4Ø9-D9).
Clinical Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is situational
X
Only required for a few select groups and only
on select drug classes
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
13 - Clinical Segment
491-VE
Diagnosis Code Count
R
Maximum count of 5
492-WE
Diagnosis Code Qualifier
R
424-DO
Diagnosis Code
R
DUR/PPS Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is situational
X
Required to receive a service fee on certain
vaccines
Field
NCPDP Field Name
Payer
Usage
Value/Comments
438-E3
Service Fee
R
441-E6
Result of Service Code
R
Vaccine
Administration:
1A
1B
1C
1D
1E
1F
1G
1H
1I
1J
1K
3N
Consultation
Services:
3A
3B
3C
3D
3E
3F
3G
3H
3J
3K
3M
3N
439-E4
Reason for Service Code
R
A valid Reason for Service Code must be
submitted
44Ø-E5
Professional Service Code
R
A valid Professional Service Code must be
submitted. For Consultation Services, use PØ.

39
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 11 of 13
Worker’s Compensation Segment
Check
Claim Billing/Claim Rebill
If Situational, Payer Situation
This Segment is situational
X
Only required for submission of a compound
claim (Field 4Ø6-D6 = 2)
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
06 – Woker’s Compensation Segment
434-DY
Date of Injury
M
CCYYMMDD
315-CF
Employer Name
RW
316-CG
Employer Street Address
RW
317-CH
Employer City Address
RW
318-CI
Employer State
RW
319-CJ
Employer Zip/Postal
Code
RW
320-CK
Employer Phone
RW
321-CR
Carrier ID
RW
435-DZ
Claim/Reference ID
RW
Claim Reversal Transaction
Transaction Header Segment
Check
Claim Reversal
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
1Ø1-A1
BIN Number
M
Same value as Claim Billing transaction
1Ø2-A2
Version/Release Number
M
DØ
1Ø3-A3
Transaction Code
M
B2
1Ø4-A4
Processor Control
Number
Same value as Claim Billing transaction
1Ø9-A9
Transaction Count
M
Maximum of 4 transactions
2Ø2-B2
Service Provider ID
Qualifier
M
Same value as Claim Billing transaction
2Ø1-B1
Service Provider ID
M
Same value as Claim Billing transaction
4Ø1-D1
Date of Service
M
Same value as Claim Billing transaction
11Ø-AK
Software
Vendor/Certification ID
M
Use value for Switch’s requirements or send
spaces
Insurance Segment
Check
Claim Reversal
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments

© 2024 Select Health. All rights reserved. 1490973 03/24
40
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 12 of 13
111-AM
Segment Identification
M
Ø4 – Insurance Segment
3Ø2-C2
Cardholder Id
M
Same value as Claim Billing transaction
Claim Segment
Check
Claim Reversal
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø7 – Claim Segment
455-EM
Prescription/Service
Reference Number
Qualifier
M
1 – Rx Billing
4Ø2-D2
Prescription/Service
Reference Number
M
Same value as Claim Billing transaction
436-E1
Product/Service ID
Qualifier
M
Same value as Claim Billing transaction
4Ø7-D7
Product/Service ID
M
Same value as Claim Billing transaction
4Ø3-D3
Fill Number
RW
Required when multiple fills of the same
Prescription/Service Reference Number (4Ø2-
D2) occur on the same day
3Ø8-C8
Other Coverage Code
RW
Same value as Claim Billing transaction
Pricing Segment
Check
Claim Reversal
If Situational, Payer Situation
This Segment is always sent
X
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
11 – Pricing Segment
43Ø-DU
Gross Amount Due
R
Same value as Claim Billing transaction
Coordination of Benefits/Other
Payments Segment
Check
Claim Reversal
If Situational, Payer Situation
This Segment is situational
X
Required only for secondary, tertiary, etc. claims
Field
NCPDP Field Name
Payer
Usage
Value/Comments
111-AM
Segment Identification
M
Ø5 – Coordination of Benefits/Other
Payments Segment
337-4C
Coordination of
Benefits/Other Payments
Count
M
Maximum count of 9
338-5C
Other Payer Coverage
Type
M
Same value as Claim Billing transaction

© 2024 Select Health. All rights reserved. 1490973 05/24
41
PROVIDER REFERENCE MANUAL: PHARMACY PLANS
MARCH 2024
APPENDIX: PAYER SHEET, CONTINUED
Materials reproduced with the consent of ©National Council for Prescription Drug Programs, Inc. 2Ø1Ø NCPDP
Last Updated January 1, 2024 Page 13 of 13
Testing Information
Test BIN
8ØØØØ8
Test PCN
DØTEST
SelectHealth is the primary insurer for this test patient
Cardholder ID
8ØØØØØØØØ
Person Code
ØØØ
Patient Name
Fred Select
Patient Date of Birth
11/15/1958
Relationship
1 – Cardholder
Gender
1 – Male
SelectHealth is the secondary insurer for this test patient
Cardholder ID
8ØØØØØØØØ
Person Code
ØØ1
Patient Name
Sally Select
Patient Date of Birth
Ø3/Ø8/196Ø
Relationship
2 – Spouse
Gender
2 – Female
